As a Cancer Voice and patient advocate I attended the Macmillan Cancer Voices Conference. This is held each year in a hotel at Gatwick and runs for 2 days with plenaries, workshops and networking. The attendees are a mix of people newly affected by cancer (diagnosed or carer) together with some old stalwarts who are, like me, advocating for themselves and others. Many of us ‘old guard’ sit on various other tumour working groups, networks, research, NHS or hospital boards, Healthwatch/LINk, charity or patient groups. My aims in attending this conference is to be able to share my experience (and that of others I’m familiar with), contribute to discussions at workshops and also come away with more knowledge about new and ongoing projects. I also like to take the opportunity to share with Macmillan projects that are underway or consideration by other organisations and that perhaps they could work collaboratively or in conjunction with these others rather than reinventing the wheel.
As a Cancer Voice and patient advocate I attended the Macmillan Cancer Voices Conference. This is held each year in a hotel at Gatwick and runs for 2 days with plenaries, workshops and networking. The attendees are a mix of people newly affected by cancer (diagnosed or carer) together with some old stalwarts who are, like me, advocating for themselves and others. Many of us ‘old guard’ sit on various other tumour working groups, networks, research, NHS or hospital boards, Healthwatch/LINk, charity or patient groups. My aims in attending this conference is to be able to share my experience (and that of others I’m familiar with), contribute to discussions at workshops and also come away with more knowledge about new and ongoing projects. I also like to take the opportunity to share with Macmillan projects that are underway or consideration by other organisations and that perhaps they could work collaboratively or in conjunction with these others rather than reinventing the wheel.
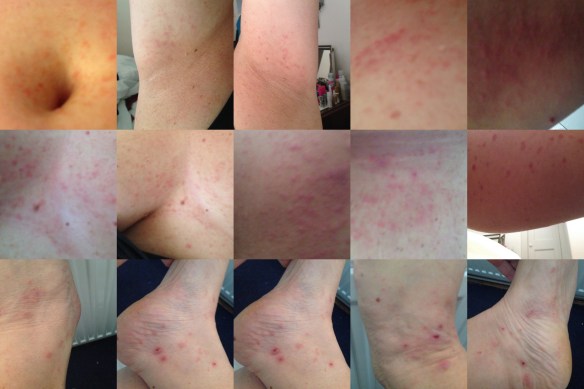
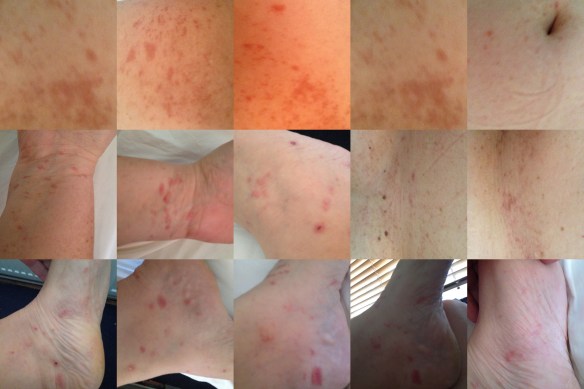
 The agenda is, as always, busy. Attending these conferences isn’t for the faint-hearted and for some can be difficult.
The agenda is, as always, busy. Attending these conferences isn’t for the faint-hearted and for some can be difficult.
I hope you find my notes from the Conference useful (my additional comments are in italic):
————————————–
Welcome from Julia Palca, Macmillan Trustee (Chairman of Board). Julia explained that she joined CancerLink in 2008 after her own diagnosis. CancerLink was taken over by Macmillan and is now known as Cancer Voices.
Why are we here today:
- “You are at the heart of everything we do”
- Cancer Voices tell us what people affected by cancer need and how they need it.
- Your Voices are influencing changes in cancer.
- Challenging times for the health service. We continue to fund-raise, deliver services and influence.
- 2012 was the most successful for fundraising. £115m raised. £112 spent on people affected by cancer. 8,000 more people reached than the year before.
- Big part of reach is our Macmillan professionals. 3,000 funded last year.
- Influence and force for change work. e.g. free social care at end of life. Welsh care delivery plan. Northern Ireland cancer commissioning plan.
Specific examples of user involvement:
Early diagnosis. A GP will only see 8 or 9 new cancer patients a year (on average). We need to raise awareness for GPs and have developed ClinRisk Tool (QCancer Overview). It has now been piloted in 500+ GP surgeries. Over 800 GPs attended training for early diagnosis.
Improve patient experience. We’ve been working toward: High quality communication patients and staff; Patients involved in decisions; and Coordinated care between settings.

 NHS National Cancer Experience Survey. Macmillan is working with partner organisations to improve on results. Cancer Voices and Healthwatch to co-create Macmillan’s guide to using the survey. Copies can be obtained from BeMacmillan.
NHS National Cancer Experience Survey. Macmillan is working with partner organisations to improve on results. Cancer Voices and Healthwatch to co-create Macmillan’s guide to using the survey. Copies can be obtained from BeMacmillan.
Campaigning for carers. 1.1m cancer carers in the UK. 50% don’t identify as carers or realise there is support available to them.
This month Macmillan are launching a new campaign to reach carers and also lobby care bill to strengthen and support carers.
Redesigning cancer care systems. Macmillan are encouraging user involvement working group as part of the programme of changes in the NHS care system.
Exciting programme ahead and a great deal of opportunities for patient/carers to get involved and improve care.
————————————–
Neil Stevens VP of Skype – keynote session.
Neil described his own experience. At the time of his diagnosis, he thought nothing of jumping on a plane for a day of meetings in Sydney and did this regularly! He was focused, impatient, driven and busy. Life was good. At the young age of 43 he noticed a lump on his hip. He was overseas on a business trip. A local Dr told him not to worry. He carried on with his business trip. Back to the UK he sought more medical advice and scans. Initially he was told it was nothing to worry about. He was fortunate to have private cover and once again pushed for more tests.
Eventually he had a diagnosis – a rare form of sarcoma – extraskeletal osteosarcoma. So he knew the name but little else.
The tumour was removed by surgery and he was back at work in 3 weeks. His life returned to ‘normal’ as if it never happened.
At a routine scan 6 weeks later life however he was told that the sarcoma was back and now in his pelvis and lungs. They stated that there were over 100 tumours in his lungs and told he probably had 18 months.
So he put on his business head. After all he was driven, focused and able. He became the Cancer Elimination Officer (CEO) of his cancer. Neil said that he had to address the cancer in the same way he addresses any business problem. He first gets all the facts and data (no small task when there is so little), he would then build a strategy to eliminate it. He was sure he would be able to do so.
He’s fortunate that he had money and contacts to track down and seek advice from the world’s expert at Sloane Kettering in the USA. When he met with them, the consultant told him ‘You can beat this’. Neil said that hearing that meant he knew it was true. Once again an incredibly positive attitude.
He started chemotherapy immediately. He knew that there was no sign of activity after round 1. He kept telling everyone he could that he would beat it. He kept a positive mind.
The final round scans couldn’t find anything!
What he learnt was the power of his own mind. He’s very factual and needed information. BUT he knew he could take control and manage it. Neil went for counselling, took up pilates, changed diet, aware of power of his own body and mindful meditation.
The hardest part was telling the children. Macmillan helped.
“Ask all the questions and let the children talk.”
He knew deep down he could do this. He knew that by addressing it as he would a business deal, he’d be able to command what he knew he needed and be in control.
He wrote a document justifying why Cyberknife should be used not radiotherapy.. he got it.
He found a trial in the US. He did a PowerPoint presentation of why he should get on the trial. He got it.
He’s now been back at work full time for a year. He’s moved to a new role which is less stressful. He believes fitness and Pilates played a part in his health. He meditates whenever he feels worried or panics. He’s learnt to keep perspective.
He did have a small relapse in June with tumours in his lungs however is now completely clear following surgery.
As with everything in his life, he wondered how he can use his experience to create change. “I was given cancer for a reason. I can do something with this.” He met with Ciaran Devane (Chief Executive at Macmillan)
Skype’s amazing and free and global. He works for Skype. What if we built a tool that allowed people with cancer connect?
Now the Skype Buddy system has been built and is being piloted. The principal is to enable people affected by cancer to be able to talk to specialists (financial counselling, medical etc) or patient to patient or carer to carer. (I’m not sure if there will be group discussions but hope there will be as it would be a great opportunity to have group chats on specific subjects with perhaps nurses or clinicians on the call too).
Digital advisory board for Macmillan that he’s putting together has representatives from the likes of Facebook, Expedia, Amazon etc.
What is Skype Buddy system? Click here for explanation.
 The system is being piloted currently and looking for people to get involved, use the system, provide feedback and evaluate.
The system is being piloted currently and looking for people to get involved, use the system, provide feedback and evaluate.
Sign up for the Skype Buddy pilot here
At present the system appears to have a small number of cancers and a limited sign up criteria. I wonder if this will be increased in order to match Buddies on better criteria. I am an Imerman Angel whereby we mentor others with the same cancer diagnosis by phone, Skype, email, letter etc, as required. I’m a little disappointed that when I spoke with a number of charities, NCAT and NHS representatives about the Imerman Angels some years ago it was dismissed as a crazy idea to ask people to use technology to speak to someone similar! Hey ho, I guess time and mindsets have moved on. Imerman Angels match us on a huge number of criteria including age, marital status, children and cancer. Although it may seem excessive, I know that some of that criteria would have been critical in my journey.
I have offered my experience to this project as I have worked with IT online projects for many years and also the Imerman Angels system (which I continue to mentor for).
We need more types of cancer in Skype Buddy project so that there is perfect matches. For example (and perhaps selfishly for me) ‘soft tissue sarcoma’ is not defined enough. Sarcoma cancer can occur anywhere in the human body and issues that may affect someone with Phyllodes in the breast will no doubt be different to someone with an Leiomyosarcoma.
Skype Buddy is about 1:1 relationship. I do hope this will open up to group chats on specific topics.
We also need to ensure the supporting Buddies are provided with good (ongoing) training. They should also be provided with the ability to reach out for support for themselves.
We need to use technology better and use it as a key element of the broader strategy.
Neil closed by saying that his views of life have changed as he enters the 2nd half of his life:
Seize the day… Enjoy the day, your life, that moment, value it. Be present with people. Engaged with people. He shared with us a very powerful statement from James Dean: “Dream as if you will live forever and live as if you will die today.”
————————————–
We then split out into different conference rooms for Welcome groups. The purpose was to meet other Cancer Voices and Macmillan team members. After introducing ourselves and finding out what each of us had done in the past 12 months for Macmillan we discussed what do we want from the conference? The main points from our group were:
- Not reinventing the wheel.
- Feedback on the projects we’re involved in.
- Updates from the previous conference.
- Sharing information, data and reports with others.
- Working collaboratively to provide information.
————————————–
Workshop – Improving Cancer Patient experience in the New NHS
Following an exercise to introduce ourselves to other Voices at our table and then a ‘ice-breaker’/competition, the workshop began.
3. Mid Staffs and the Francis Report. The final report and executive summary can be viewed here.
4. Macmillans’ work to improve cancer experience
5. Group Exercise – using tools to improve patient experience
Mid Staffs
Failings of Care at Mid Staffs – Robert Francis QC Feb 2013 stated “This is a story of appalling and unnecessary suffering of hundreds of people”. The priority of his report, he said, was not to find a scapegoat, but find ways of putting patients and the quality of care first.
- Not just cancer.. of course the mortality of all illnesses was too high at Mid Staffs.
- Waiting times for cancer patients to see specialists were far too long which meant that many people died where as they should have been saved.
- Chronic understaffing on cancer wards. Lack of commitment to improving outcomes for cancer patients.
- Obsession for reaching targets but not standard of care for living longer and better quality of life.
- No rapid referral system to oncologists which should have been in place.
- Lack of support for the clinician from the MDT surgeons.
Failings on cancer care at Mid Staffs
- Not listening sufficiently to patients and staff
- Failing to tackle a negative culture involving a tolerance of poor standards and disengagement.
- Increased focus on reaching national access targets, achieving financial balance and seeking foundation trust status.
How do we know if patient experience is good/bad?
There’s the NHS cancer patient experience survey, peer reviews and several different areas.
- Information and Support
- Emotional Support
- Holistic plan
- Dignity and respect
Francis Inquiry Report recommendations
- Transparency
- Fundamental standards
- Accountable
- Compliance
Macmillan have devised
Value Based Standard is a set of behaviours that is practical developed by patients and carers.
There are eight behaviours in the Macmillan Values Based Standard:
1. Naming – I am the expert on me.
2. Private communication – My business is my business
3. Communicating with more sensitivity – I’m more than my condition
4. Clinical treatment and decision making – I’d like to understand what will happen to me.
5. Acknowledge me if I’m in urgent need of support – I’d like not to be ignored.
6. Control over my personal space and environment – I’d like to feel comfortable.
7. Managing my own – I don’t want to feel alone on this.
8. Getting care right – my concerns can be acted upon.
Sadly a great deal of these ‘standard’ points should be what we do every day as humans. Why do we need standards to ask a medical member of staff to remember to ask how someone wants to be addressed? Anna, Ms Wallace, Miss Wallace etc.
Common courtesy!!
What is the NHS Cancer Patient Experience Survey (CPES)
The survey was completed by over 70,000 people and covers care before, during and after hospital. Does it survey the family of deceased cancer patients about their experience?
 We spent a short amount of time looking at extracts of the Survey and attempting to work out where we might feel improvement should be focused. The Survey results are lengthy and difficult to interpret. There are many tips on doing so, such as look at the figures for last year and this year to see if there has been an improvement. How does that Trust compare to other Trusts? If many Trusts performed badly, could you Trust improve sufficiently to be hailed as the ‘gold standard’?
We spent a short amount of time looking at extracts of the Survey and attempting to work out where we might feel improvement should be focused. The Survey results are lengthy and difficult to interpret. There are many tips on doing so, such as look at the figures for last year and this year to see if there has been an improvement. How does that Trust compare to other Trusts? If many Trusts performed badly, could you Trust improve sufficiently to be hailed as the ‘gold standard’?
In the final minutes of the workshop we discussed what we might do as patient/carers/advocates to ‘encourage’ our local Trusts to improve, with measurable improvement and to be held account.
I had been booked into a workshop by Healthtalkonline. Disappointed that they weren’t in attendance at the conference as I wanted to find out first hand more about their work, strategy and future plans. Perhaps next year?
————————————–
The first day of Conference ended with a networking opportunity via drinks and then dinner. It is always a joy to meet up with friends at this Conference, many of whom I don’t see from year to year (except on social media). This year the entertainment was provided by a singer who crooned his way through a whole host of fabulous tunes. On our table we seemed to know all the words and were (I think) the first ones up for a little dance! Great fun and perfect entertainment for this event as it appealed to pretty much every age group (the joy of Robbie Williams doing covers!).
————————————–
The second day began with the second workshop of the conference.
Workshop – Commissioning the bigger picture
What is commissioning?
- Purchase/buying services.
The theory is that we are all commissioners.
- I’m buying for my needs. I look for value for money, choice, what I need, who am I buying for, can we afford it and quality.
Health service commissioning is similar. It happens all the time. Some stuff will be bought every week. some things might be purchased for special occasion.
The commissioning cycle.
Assessing needs -> Needs assessment -> Planning -> Specifying -> contracting -> evaluation.
Clinical Commissioning Groups (CCG) now do the ‘buying’ of services in the new NHS.
- CCGs are a group of GPs that come together to form a group to commission services.
- No boundaries are set as to how many GPs are required or the maximum number either.
- There are now over 200 CCGs.
- £100bn is the NHS budget and £65bn of which goes to the CCG.
Do GPs know what to buy? How are these different CCGs going to ensure that nothing slips between the geographical groups of CCGs?
Kings Fund video – An alternative guide to the new NHS in England.
Sadly we didn’t get to see it as the broadband was too slow.. perhaps it should have been downloaded prior to the conference to play locally?
We then worked (as best we could) through picture handout (final slide of video below – click to enlarge).
All organisations involved have a duty. Briefly, who is involved?
- Public Health England – more proactive, awareness and prevention (sit within the council – local government.
- Social care – care of the elderly, supporting people with disabilities, someone post cancer treatment needing assistance at home.
- Health & Wellbeing boards – brings together main leaders in particular area.
- Healthwatch – responsible for supporting public voice in monitoring health and social care locally.
- Cancer Commissioning. Commissioning Support Units support the CCGs and, in the most part, are made up of the original ‘commissioners’ in the old NHS structure.
HOWEVER one of the significant rules for CCGs is that they have to engage with members of the public.
Most of these are linked to the clinical senates within the new strategic clinical networks
How can you influence what is happening locally?
- Clinical Commissioning Groups,
- Patient Participation Groups – ask for information at your local GP surgery.
- Hospital boards – find out which boards have patient representation.
- Health and wellbeing boards making decisions about the needs of the local area.
- Healthwatch/LINk
Or at a regional level. Make enquiries. Ask where you can be involved.
If interested in cancer commissioning get involved with strategic clinical network.
Not sure where to start? How do you get involved?
Start with Macmillan involvement coordinators who can advise on where to go.
A useful 7 point ‘reminder’ for consideration and preparation before going into any patient involvement group or meeting:
- Define your preferred outcome and retreat outcome
- Consider the second position – what does the other person think?
- Be clear with benefits for both sides
- Present evidence and proof to reassured
- Think about your delivery
- Anticipate barriers or blockages
- Explore the barrier, empathise, re-present.
————————————–
My final workshop of the conference was on a subject I’m passionate about. I hoped to find out more about initiatives that Macmillan are involved in to improve care for people living beyond diagnosis.
Workshop: Improving Care for people living with and beyond cancer
Sandra Rowlands and Gloria Payne
National Cancer Survivorship Initiative (NCSI):
Survivorship being from the first thought of cancer until the last breath… not just post treatment or for a set period of time.
Recovery Package:
They showed a slide to show the numbers of people living with cancer and how they are projected to boom:
- In 2010 there were 220,000 living with and beyond cancer.
- In 2030 it is projected that there will 370,000 (1 yr survival); 570,000 to 990,0000 (1-5 yrs) and 1,290,000 – 2,680,000 (more than 5 years).
Often it is spoken about that the number of people living with cancer is set to double by 2030.
We are already struggling to accommodate the increased numbers of cancer patients. If the numbers are correct we need to be collaboratively working for survivorship – charities, NHS, local health, patient groups etc.
Another projected figure that truly is worrying is that by 2020 almost 50% of Britons will get cancer but 38% will not die FROM cancer.
38.7% of cancer survivors are of working age ie 18-64 = 38.7% If this percentage of working people living with a cancer diagnosis continues at almost 50% of the population then it will have a huge impact because of needs and use.
Median survival times are improving. 1971-72 = 1 year whereas 2007 5.8 years.
NCSI 2010 Vision
There are five key shifts:
- Cultural – focus on recovery, health and wellbeing.
- Holistic assessment 9 individual and personalised care planning.
- Self management – not clinical follow up.
- Tailored follow up support.
- Patient Reported Outcomes Measures (PROMS) not clinical activity.
My cancer treatment – gives national cancer experience survey results, and peer reviews, what hospitals are centre of excellence, mortality rates and survival rates etc.
New document prepared by the NCSI “Living With and Beyond Cancer: Taking action to improve outcomes 2013“.
Also detailed is a Recovery package to support the new NHS commissioning and includes:
- Supporting self management.
- Physical activity and healthy lifestyle.
- Information financial and work support.
- Managing consequences of treatment.
- Assessment and care planning.
- Treatment summary and cancer care review.
- Health and wellbeing event.
Macmillan Identifying your concerns checklist (white form) which is completed by the patient/carer and then returned to the specialist (holistic needs assessment).
This is then discussed and worked through with the Care plan which then has a plan of action etc.
There is an excellent piece on the NCSI website which explains each part and also has downloadable forms to adopt for good practice.
These are also available on the BeMacmillan website.
A useful tip for the Treatment Summary use was for the purpose of travel insurance. As any cancer patient knows travel insurance can often be difficult and expensive to find. Macmillan advised that the Treatment Summary form could be used as the basis of medical information for this purpose. My own travel insurance is through InsuranceWith who specialise in travel insurance for people with long term conditions.
We spoke about the importance of Health and wellbeing events being held locally. It was suggested that through the patient participation groups this could be set up and achieved. Also to contact your Macmillan Involvement Coordinator to assist and perhaps provide some funding.
In order to sustain recovery, perhaps via self care with support and open access to the medical teams. Shared care within the hospital environment and local, social and self care. However complex cases must be managed through an MDT.
Care co-ordination and remote surveillance. This needs collaborative working between the clinical setting and local/social care together with third sector organisations.
Walking for health is a scheme whereby walks are organised for free locally. However could more be done. If you have high blood pressure or a heart complaint you are entitled to some physical exercise grant/access however as a cancer patient there is no physical exercise grant/access available yet. This should be highlighted.. could you raise this with your MP?
Work and cancer – Often this is overlooked during treatment but essential for so many to be able to return to work in some capacity. Macmillan advise people NOT to resign but to find a working solution with your employer.
Taking action – Innovation to implementation: Stratified pathways of care for people living with or beyond cancer- A “how to guide” was published by NHS improvement in 2013, and provides local teams with a very practical ‘how to’ guide based on the experience of the test sites.
What does success look like?
- Improved outcomes for people living with and beyond cancer.
Can you help ensure that this happens?
————————————–
The final plenary session, “A journey with a view from 3 sides of the fence”, and close for the Conference was given by Johnny Browne who was a GP, was a carer for his wife with cancer and is a Macmillan GP advisor for Northern Ireland.
Macmillan GPs special interest in cancer and their role is to promote best cancer care in their area/locality. (Macmillan fund GP training and I would love to know which GPs had received the training so that if I was to move locality I could ensure my GP was familiar with cancer treatments. Is the list of Macmillan GPs available to the public? I can’t find it!)
In an attempt to point out areas where I think cancer care can be improved and looking from 3 very different perspectives:
- Do not forget as a GP the importance of self esteem and body image in cancer patients.
- Look Good.… Feel Better programme
- Diagnosing cancer early:
- Awareness
- Difficult journey, sometimes truly difficult, often symptoms mask as something else. Patients should be aware of symptoms and not be afraid or embarrassed to say anything. “If you were meant to be shot, you’ll not drown”
- Diagnosing Earlier App?
- Take pity on the poor GP who is like a penguin. Don’t refer too many patients. Make sure all your referrals meet the referral guidelines?
- All cancer studies ask “how many times you attended the GP before diagnosis”
- Most of the time the GP didn’t miss anything as often symptoms can be something else too… but we’re improving in seeing patterns.
- Improve communication
- As a carer I realised how important it was. Written communication and results. Between patients, medics, staff, GP etc etc
- How many people do you get in contact with during your cancer journey?
- Sensitivity, know your patient, what they want, how they should be addressed etc.
- Difficult for me as a GP to navigate the cancer journey. It can be extremely difficult for someone who is new to the NHS and ‘cancerland’.
- Treatment summary – Macmillan have developed this and it explains what happened to the patient. 3 copies – patient, hospital and GP. You can take this with you in the case of emergency, insurance or advice.
- Twitter showing how the world really looks from his photos posted. (Commander Hadfield)
- #hellomynameis campaign on Twitter
- Four things I’ve learnt about communication
- Health care professionals can do better.
- Look patients in the eye
- Difficult care pathway – passport to death. Talked to the patient to obtain the information rather than GO through a form. People and organisations have made the form more important than the patient – we need to change that back and hear the story rather than fill the form.
- 1 or 2% who give you bad communication can undo all the good of the rest of the team who give great communication.
- When you are going through you cancer journey, we don’t or are reluctant to complain.
- Perhaps it’s up to us to put the message out there or complain for others (factually, professionally and politely).
- Spread the word ‘Living with Cancer’
- I knew nothing as a GP nor as a carer but as a Macmillan GP I do… from you.
- All cancer patients need follow up and review.
- Travel insurance for those affected by cancer.
- Remember to live.. we did House building in Zambi, white water rafting and more… remember to Live.
- Don’t remove Hope.
- Why can’t you be one of the small survival percent.
- Spread the word about exercise
- Any exercise is good.
- Remember no one should face cancer alone.
- Keep a diary.
- Not of medical things but also happy fun memories and thoughts. It can be a lonely disease even with family and friends.
General Practice 2013.
Its changing. How does someone with a chronic condition have a relationship with the GP? It’s in change or flux.
GP out of Hours 2013.
Important to a cancer patient to be able to access GPs out of hours. Could they avoid the A&E admissions?
But A&E is often not a great place for a cancer patient to be first hand and stuck on a bed in a hallway. We need to get quicker access.
In his wife, Lynda’s diary was a note:
“I hope you enjoy your new job with Macmillan to help people with cancer and to bring your personal experience to this”.
————————————–
General comments for this Conference:
Time is short to discuss fully all the topics and workshops and listen to the plenaries. Perhaps we should consider:
1/ Sending out by email or post preliminary information for reading prior to the Conference.
2/ All Voices are attending to participate. I don’t think there’s a need for an ‘ice-breaker’ in each session. It just wastes time and irritates those who want to get on with the discussion.
3/ Whilst all Voices attending have a personal experience of cancer (diagnosed or as a carer) it should be encouraged to, if required, use snippets of their experience if pertinent to the workshop.
4/ Should some of the workshops be for newbies and some for ‘old stalwarts’?
5/ Should there be a workshop on ‘how to complain’ so that many of the ‘negative’ experiences that participants feel they need to share can be addressed in this workshop in a constructive manner?
6/ So often during the conference people bring up negative experiences and complaints with the health system. Could Macmillan also encourage people to report when things have gone well and encourage best practice by highlighting that someone has excelled at their job! We all like to be appreciated and there are a great many people doing a fantastic job in the NHS and cancerland – we must learn to say thank you!